The original press release from The University of Chicago, by Carla Reiter, can be read here.
Ideally, injectable or implantable medical devices should not only be small and electrically functional, they should be soft, like the body tissues with which they interact. Scientists from two University of Chicago (UofC) labs set out to see if they could design a material with all three of those properties. The material they devised, with an assist from the X-ray Science Division 12-ID-B and 32-ID-B.C x-ray beamlines at the U.S. Department of Energy’s Advanced Photon Source, and from the Argonne Center for Nanoscale Materials (CNM), forms the basis of an ingenious light-activated injectable device that could eventually be used to stimulate nerve cells and manipulate the behavior of muscles and organs. Their results, and that of their co-authors from The University of Chicago, Northwestern University, Argonne National Laboratory, and the University of Illinois at Chicago were published in Nature Materials.
“Most traditional materials for implants are very rigid and bulky, especially if you want to do electrical stimulation,” said Bozhi Tian, an assistant professor in chemistry at the University of Chicago, whose lab collaborated with that of UofC neuroscientist Francisco Bezanilla, the Lillian Eichelberger Cannon Professor of Biochemistry and Molecular Biology.
The new material, in contrast, is soft and tiny, composed of particles just a few micrometers in diameter—far less than the width of a human hair—that disperse easily in a saline solution so they can be injected. The particles also degrade naturally inside the body after a few months, so no surgery would be needed to remove them.
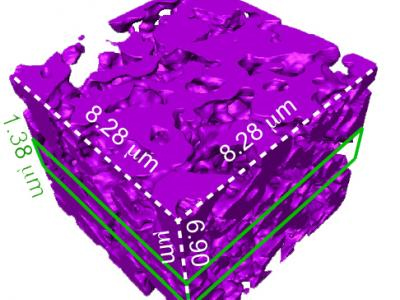
Each particle is built of two types of silicon that together form a structure full of nanoscale pores, like a tiny sponge. And like a sponge, it is also squishy—a hundred to a thousand times less rigid than the familiar crystalline silicon used in transistors and solar cells. “It is comparable to the rigidity of the collagen fibers in our bodies,” said Yuanwen Jiang, Tian’s graduate student. “So we’re creating a material that matches the rigidity of real tissue.”
The material constitutes half of an electrical device that creates itself spontaneously when one of the silicon particles is injected into a cell culture, or, eventually, a human body. The particle attaches to a cell, making an interface with the cell’s plasma membrane. Those two elements together—cell membrane plus particle—form a unit that generates current when light is shined on the silicon particle.
“You don’t need to inject the entire device; you just need to inject one component,” said João L. Carvalho-de-Souza, a postdoctoral scholar in Bezanilla’s lab. “This single particle connection with the cell membrane allows sufficient generation of current that could be used to stimulate the cell and change its activity. After you achieve your therapeutic goal, the material degrades naturally. And if you want to do therapy again, you do another injection.”
The scientists built the particles using a process they call nano-casting. They fabricate a silicon dioxide mold composed of tiny channels, or “nano-wires,” about seven nanometers in diameter and connected by much smaller “micro-bridges.” Into the mold they inject silane gas, which fills the pores and channels and decomposes into silicon. The focused ion beam (FIB) lithography instrument and FIB expertise of the CNM was used in the preparation of the unique mesoporous material for the various microscopy techniques used in this paper, including atom probe tomography and transmission x-ray microscopy. CNM was also responsible for fabrication of the optical masks by using the laser pattern generator for SU-8 patterning.
And this is where things get particularly cunning. The scientists exploit the fact the smaller an object is, the more the atoms on its surface dominate its reactions to what is around it. The micro-bridges are minute, so most of their atoms are on the surface. These interact with oxygen that is present in the silicon dioxide mold, creating micro-bridges made of oxidized silicon gleaned from materials at hand. The much larger nano-wires have proportionately fewer surface atoms, are much less interactive and remain mostly pure silicon.
“This is the beauty of nanoscience,” Jiang said. “It allows you to engineer chemical compositions just by manipulating the size of things.”
Finally, the mold is dissolved. What remains is a web-like structure of silicon nano-wires connected by micro-bridges of oxidized silicon that can absorb water and help increase the structure’s softness. The pure silicon retains its ability to absorb light.
The scientists have added the particles onto neurons in culture in the lab, shone light on the particles, and seen current flow into the neurons which activates the cells. The next step is to see what happens in living animals. They are particularly interested in stimulating nerves in the peripheral nervous system that connect to organs. These nerves are relatively close to the surface of the body, so near-infra-red wavelength light can reach them through the skin.
Tian imagines using the light-activated devices to engineer human tissue and create artificial organs to replace damaged ones. Currently, scientists can make engineered organs with the correct form but not the ideal function.
To get a lab-built organ to function properly, they will need to be able to manipulate individual cells in the engineered tissue. The injectable device would allow a scientist to do that, tweaking an individual cell using a tightly focused beam of light like a mechanic reaching into an engine and turning a single bolt. The possibility of doing this kind of synthetic biology without genetic engineering is enticing.
“No one wants their genetics to be altered,” Tian said. “It can be risky. There’s a need for a non-genetic system that can still manipulate cell behavior. This could be that kind of system.”
See: Yuanwen Jiang1, João L. Carvalho-de-Souza1, Raymond C.S.Wong1, Zhiqiang Luo1, Dieter Isheim2, Xiaobing Alan W. Nicholls4, Il Woong Jung3, Jiping Yue1, Di-Jia Liu3, Yucai Wang1, Vincent De Andrade3, Xianghui Xiao3, Luizetta Navrazhnykh1, Dara E.Weiss1, XiaoyangWu1, David N. Seidman2, Francisco Bezanilla1*, and Bozhi Tian1**, “Heterogeneous silicon mesostructures for lipid-supported bioelectric interfaces,” Nat. Mater., Advance online publication (27 June 2016). DOI: 10.1038/NMAT4673
Author affiliations: 1The University of Chicago, 2Northwestern University, 3Argonne National Laboratory, 4University of Illinois at Chicago
Correspondence: *[email protected], **[email protected]
This work is supported by the Air Force Office of Scientific Research (AFOSRFA9550-14-1-0175, FA9550-15-1-0285), the National Science Foundation (NSF CAREER, DMR-1254637; NSF MRSEC, DMR 1420709), the Searle Scholars Foundation, the National Institutes of Health (NIH GM030376), and The University of Chicago Start-up Fund. A portion of this work was performed at the Center for Nanoscale Materials, a U.S. Department of Energy (DOE) Office of Science-Basic Energy Sciences User Facility under Contract No. DE-AC02-06CH11357. This research used the resources of the Advanced Photon Source, a U.S. DOE Office of Science User Facility operated for the DOE Office of Science by Argonne National Laboratory under Contract No. DE-AC02-06CH11357.
Argonne National Laboratory is supported by the Office of Science of the U.S. Department of Energy. The Office of Science is the single largest supporter of basic research in the physical sciences in the United States, and is working to address some of the most pressing challenges of our time. For more information, please visit science.energy.gov.